INSOMNIA(Poor Sleep)
About one in five people has some difficulty with sleeping. However, there are many things you can do to help yourself. This leaflet aims to show you some of them. For example, simple things like winding down before bedtime, avoiding certain foods and drinks, and a bedtime routine can help. Further ways to promote sleep in more difficult cases include relaxation techniques, regular exercise, and behavioural and cognitive therapies. Sleeping tablets are not the best way to help with sleep problems because you can get addicted to them, and they often stop working if you take them regularly.
Normal sleep
A normal night's sleep has three main parts:
- Quiet sleep. This is divided into stages 1-4. Each stage becomes more 'deep'. Quiet sleep is sometimes called deep sleep.
- Rapid Eye Movement (REM) sleep. REM sleep is when the brain is very active, but the body is limp, apart from the eyes which move rapidly. Most dreaming occurs during REM sleep.
- 3. Short periods of waking for 1-2 minutes.
Each night, about 4-5 periods of quiet sleep alternate with 4-5 periods of REM sleep. In addition, several short periods of waking for 1-2 minutes occur about every two hours or so, but occur more frequently towards the end of the night's sleep. The graph below shows a typical normal pattern of sleep in a young adult.
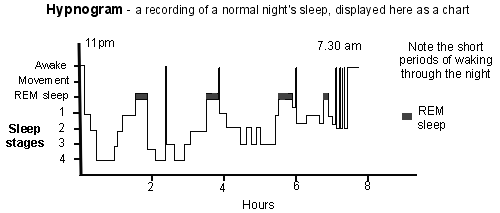
Normally, you do not remember the times that you wake if they last less than two minutes. If you are distracted during the wakeful times (for example, a partner snoring, traffic noise, etc), then the wakeful times tend to last longer, and you are more likely to remember them.
What is insomnia?
Insomnia means poor sleep. About one in five adults does not get as much sleep as they would like. Poor sleep can mean:
- Not being able to get off to sleep.
- Waking up too early.
- Waking for long periods in the night.
- Not feeling refreshed after a night's sleep.
If you have poor sleep, you may be tired in the daytime, have reduced concentration, become irritable, or just not function well.
What is a normal amount of sleep?
Different people need different amounts of sleep. Some people function well and are not tired during the day with just 3-4 hours' sleep a night. Most people need more than this. Six to eight hours per night is average. Most people establish a pattern that is normal for them in their early adult life. However, as you become older, it is normal to sleep less. Many people in their 70s sleep less than six hours per night.
So, everyone is different. What is important is that the amount of sleep that you get is sufficient for you, and that you usually feel refreshed and not sleepy during the daytime. Therefore, the strict medical definition of insomnia is ...'difficulty in getting to sleep, difficulty staying asleep, early wakening, or non-restorative sleep despite adequate time and opportunity to sleep, resulting in impaired daytime functioning, such as poor concentration, mood disturbance, and daytime tiredness'.
The causes of poor sleep?
Poor sleep may develop for no apparent reason. However, there are a number of possible causes which include the following:
Concern about wakefulness
You may remember the normal times of being awake in the night. You may feel that to wake in the night is not normal, and worry about getting back off to sleep. You may 'clock watch', and check the time each time you wake up. This may make you irritated or anxious, and you are more likely to remember the times of wakefulness. You may then have an impression of having a bad night's sleep, even if the total amount of time asleep was normal.
Temporary problems
Poor sleep is often temporary. This may be because of stress, a work or family problem, jet-lag, a change of routine, a strange bed, etc. Poor sleep in these situations usually improves in time.
Anxiety or depression
You may find it difficult to switch off your anxieties about work, home or personal problems. Also, poor sleep is sometimes due to depression. Other symptoms of depression include: a low mood, lethargy, poor concentration, tearfulness, and persistent negative thoughts. Depression is common. Treatment of depression or anxiety often cures the poor sleep too.
Sleep apnoea
This sometimes occurs in people who snore, most commonly in obese people. In this condition the large airways narrow or collapse as you fall asleep. This not only causes snoring, but also reduces the amount of oxygen that gets to the lungs. This causes you to wake up to breathe properly. You may wake up many times each night which may result in daytime tiredness.
Other illnesses
Various illnesses keep some people awake. For example, illness causing pain, leg cramps, breathlessness, indigestion, cough, itch, hot flushes, mental health problems, etc.
Stimulants
These can interfere with sleep. There are three common culprits:
- Alcohol - many people take an alcoholic drink to help sleep. Alcohol actually causes broken sleep and early morning wakefulness.
- Caffeine - which is in tea, coffee, some soft drinks such as cola, and even chocolate. It is also in some painkiller tablets and other drugs. Caffeine is a stimulant and may cause poor sleep.
- Nicotine - (from smoking) is a stimulant.
Street drugs
For example, ecstasy, cocaine, cannabis and amfetamines (amphetamines) can affect sleep.
Prescribed drugs
Some drugs sometimes interfere with sleep. For example, diuretics ('water tablets'), some antidepressants, steroids, beta blockers, some slimming tablets, painkillers containing caffeine, and some cold remedies containing pseudoephedrine. Also, if you suddenly stop taking regular sleeping tablets or other sedative drugs, this can cause 'rebound' poor sleep.
Unrealistic expectations
Some people just need less sleep than others. If your sleep pattern has not changed, and you do not feel sleepy during the day, then you are probably getting enough sleep. Older people and people who do little exercise tend to need less sleep. Some people think they should be able to nap during the day - and sleep eight hours at night!
A vicious cycle
Whatever the initial cause, worry about poor sleep, and worry about feeling tired the next day, are common reasons for the problem to become worse.
Poor sleep (insomnia) can be classified into the following categories:
- Primary insomnia is insomnia that occurs when no illness or other secondary cause is identified. Primary insomnia accounts for about one in five cases of long-term insomnia.
- Secondary insomnia is when insomnia occurs as a symptom of, or is associated with, other conditions. These can be medical or mental health conditions, or drug or substance misuse.
- Short-term if insomnia lasts between one and four weeks.
- Long-term (or persistent) if insomnia lasts for four weeks or longer.
To help improve poor sleep?

It is often helpful to understand that short periods of waking each night are normal. Some people are reassured about this and so do not become anxious when they find themselves awake in the night. Also, remember that worry about poor sleep can itself make things worse. Also, it is common to have a few bad nights if you have a period of stress, anxiety or worry. This is often just for a short time and a normal sleep pattern often resumes after a few days.
General tips for sleeping better (often called 'Sleep Hygiene')
- Reduce caffeine - do not have any food, drugs, or drinks that contain caffeine or other stimulants for six hours before bedtime.
- Do not smoke within six hours before bedtime.
- Do not drink alcohol before bedtime.
- Do not have a heavy meal just before bedtime.
- Do not do any strenuous exercise within four hours of bedtime.
- Body rhythms - try to get into a routine of wakefulness during the day, and sleepiness at night. The body becomes used to rhythms or routines. If you keep to a pattern, you are more likely to sleep well. Therefore:
- No matter how tired you are, do not sleep or nap during the day.
- It is best to go to bed only when sleepy-tired in the late evening.
- Switch the light out as soon as you get into bed.
- Always get up at the same time each day, seven days a week, however short the time asleep. Use an alarm to help with this. Resist the temptation to 'lie-in' - even after a poor night's sleep. Do not use weekends to 'catch up' on sleep, as this may upset the natural body rhythm that you have got used to in the week.
- The bedroom should be a quiet, relaxing place to sleep.
- It should not be too hot, cold, or noisy.
- Earplugs and eye shades may be useful if you are sleeping with a snoring or wakeful partner.
- Make sure the bedroom is dark with good curtains to stop early morning sunlight.
- Don't use the bedroom for activities such as work, eating or television.
- Consider changing your bed if it is old, or not comfortable.
- Hide your alarm clock under your bed. Many people will 'clock watch' and this does not help you to get off to sleep.
- Mood and atmosphere - try to relax and 'wind down' with a routine before going to bed. For example:
- A stroll followed by a bath, some reading, and a warm drink (without caffeine) may be relaxing in the late evening.
- Do not do anything that is mentally demanding within 90 minutes of going to bed - such as studying.
- Go to bed when sleepy-tired.
- Some people find playing soft music is helpful at bedtime. Try a player with a time switch that turns the music off after about 30 minutes.
- If you cannot get off to sleep after 20-30 minutes - then get up. Go into another room, and do something else such as reading or watching TV rather than brooding in bed. Go back to bed when sleepy. You can repeat this as often as necessary until you are asleep.
Relaxation techniques
These aim to reduce your mental and physical arousal before going to bed.
Daytime exercise
Regular daytime exercise can help you to feel more relaxed and tired at bedtime. This may help you to sleep better.
Behavioural and cognitive therapies
Research studies have found that behavioural and cognitive therapies will improve sleep in adults with insomnia.
There are various types or therapy and include the following:
- Stimulus-control therapy - This helps you to re-associate the bed and bedroom with sleep, and to re-establish a consistent sleep/wake pattern.
- Sleep restriction therapy - The principle of this treatment is that you limit the time that you spend in bed at night. As things improve, the time in bed is then lengthened.
- Relaxation training - This teaches you ways of reducing tension. For example, this may include the progressive muscle relaxation technique.
- Paradoxical intention - This involves staying passively awake, avoiding any intention to fall asleep. Its use is limited to people who have trouble getting to sleep (but not maintaining sleep).
- Biofeedback - This provides visual or auditory feedback to help you control certain body functions (such as muscle tension).
- Cognitive therapy - Briefly, cognitive therapy is based on the idea that certain ways of thinking can trigger or 'fuel' certain health problems, such as poor sleep. The therapist helps you to understand your thought patterns. In particular, to identify any harmful or unhelpful ideas or thoughts which you have that can contribute to your not sleeping well. The aim is then to change your ways of thinking and/or behaviour to avoid these ideas. Also, to help your thoughts to be more realistic and helpful. Cognitive therapy is often used in combination with a behavioural intervention (such as stimulus control, sleep restriction, or relaxation training); this is then called cognitive behavioural therapy - or CBT.
Sleeping tablets
Note: Sleeping tablets are not usually advised
The main types of sleeping tablets are in a class of drugs called benzodiazepines. In the past, sleeping tablets were commonly prescribed. However, they have been shown to have problems, and are now not commonly prescribed.
Possible problems with sleeping tablets include:
- Drowsiness the next day. You may not be safe to drive or to operate machinery.
- Clumsiness and confusion in the night if you have to get up. For example, if you have had a sleeping tablet, you may fall over if you get up in the night to go to the toilet.
- Tolerance to sleeping tablets may develop if you take them regularly. This means that, in time, the usual dose has no effect. You then need a higher dose to help with sleep. In time, the higher dose then has no effect, and so on.
- Some people become dependent (addicted) on sleeping tablets, and have withdrawal symptoms if the tablets are stopped suddenly.
Sometimes a sleeping tablet is advised
If a sleeping tablet is prescribed, it is usually just a short course (a week or so) to get over a particularly bad patch. Sometimes a doctor will advise sleeping tablets to be taken on only two or three nights per week, rather than on every night. This prevents tolerance or dependence to the tablet from developing.
Note: See a doctor if you feel that illness or medication is causing poor sleep. Treating any underlying condition that is causing the problem, if possible, can help to promote sleep. In particular, depression and anxiety are common causes of poor sleep and can often be treated.

 INSOMNIA
INSOMNIA

